- Home
- About
- Programs
- Pain Help Now
- News
- Locations
- Contact
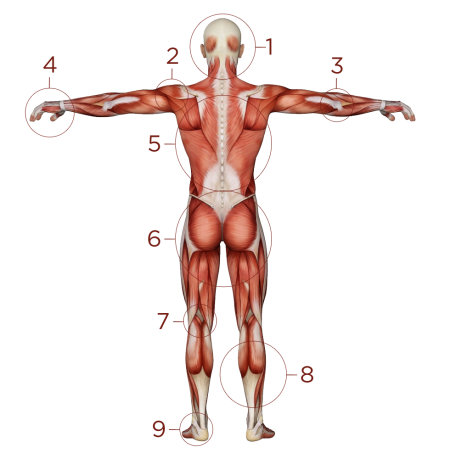
The first step to treating the pain is locating the pain
Whiplash-Associated Disorder (WAD)
The term “whiplash-associated disorder” is used to describe the clinical manifestations of a whiplash injury – which occurs when an “acceleration-deceleration” force is applied on the neck. The neck is injured by a sudden jerking or “whipping” of the head – straining the muscles and ligaments of the neck beyond their normal range of motion. While many associate the occurrence of WAD with car accidents, it can occur in any mishap when an acceleration-deceleration force is applied on the neck for example, in a diving accident, on roller coasters, sports injuries, or being punched or shaken.
Symptoms:
– Pain in the neck, head, shoulder, and arms
– Pain and stiffness in the neck – muscles may feel knotted and stiff
– Pain when moving head from side-to-side, front-to-back, and rotation
– Tenderness
– Headaches
Neck Pain
Our necks are exposed to a lot of stress. Often, people experience pain in this region caused by a number of different factors. The pain may begin in any of the structures in the neck (muscles, nerves, vertebrae and the disks between them, etc.) and can radiate down to the back and arms. Pain can also be radiated from other areas like the shoulder, jaw, head, or upper arms. A common cause of neck pain is muscle strain or tension – and everyday activities are the culprit. Being bent over a desk all day, poor posture while reading or watching TV, or sleeping in an awkward position can all be causes. It can also be caused by more serious incidents, like falls or accidents. Other causes may include a cervical herniated disk, arthritis, and meningitis.
Symptoms:
– Stiffness and soreness of the neck
– Headaches
– Difficulty moving head
– Pain that spreads to shoulders, arms, or back
– If neck pain involves nerves, you may feel numbness, tingling, or weakness in your arm, hand, or elsewhere
Frozen Shoulder (Adhesive Capsulitis)
Frozen shoulder is the common name of adhesive capsulitis, an inflammatory condition that restricts motion in the shoulder. The tissues around the joint stiffen, adhesions (internal scar tissue) form, and shoulder movements become difficult and painful. The condition sometimes occurs because of lack of use due to pain caused by injury, but can also arise with no obvious cause. Those associated with an increased risk for this condition include those with diabetes, shoulder trauma (including surgery), hyperthyroidism, and a history of open heart disease or cervical disk disease.
Symptoms:
– Stiffness
– Pain
– Limited Motion
AC Joint Seperation
The shoulders are the most mobile joints in the body, but unfortunately this makes them prone to injury. A shoulder separation is the partial or complete separation of the clavicle (collarbone) and the acromion process (the top of the shoulder blade at the end) which meet at what is called the acromioclavicular joint (AC joint). The most common cause of a separated shoulder is a fall or blow to the shoulder. The impact may stretch or tear the ligaments that stabilize the AC joint. This separates the bones in the shoulder, creating a bump at the top of the shoulder.
Symptoms:
– Intense shoulder pain
– Tenderness of the shoulder and collarbone
– Shoulder or arm weakness
– Shoulder bruising or swelling
– Limited shoulder movement
– A bump at the top of the shoulder
Tennis Elbow
Lateral epicondylitis, also known as “tennis elbow,” is an overuse syndrome. There is pain or inflammation on the outside of the forearm near the elbow. The tendon, which connects muscle to bone, might be partially torn at or near the place where it connects to the bony bump on the outside of the elbow (called the lateral epicondyle). Tennis elbow most commonly affects people in their dominant arm, but it can occur in either or both arms. Tennis elbow is caused by repeated motions of the wrist or forearm. The injury is called “tennis elbow” because of its common occurrence in the sport. The violent extension of the wrist, like during a backhand hit, causes the condition. However, any activity that involves repetitive twisting of the wrist, like using a screwdriver, is also responsible.
Symptoms:
– Elbow pain that gradually worsens
– Weak grasp
– While grasping or twisting, pain radiates from the outside of the elbow to the forearm and back of the hand when grasping or twisting
Golfers Elbow
This condition, also known as medial epicondylitis, is a very similar injury to tennis elbow, but on the inside of the elbow. Due to overuse, the tendon tears near the region where it connects to the bony bump on the inside of the elbow (called the medial epicondyle). As with tennis elbow, a variety of people experience this injury. Athletes who use their wrists or clench their fingers repeatedly can develop this condition. It is caused by damage to the muscles and tendons that control the wrist and fingers. The damage is caused by repetitive or excess stress on the wrist and fingers. Activities like golf, throwing sports (pitching), racket sports, and simple things like typing, hammering, or painting can lead to this injury.
Symptoms:
– Pain and tenderness on the inner side of the elbow
– Pain radiating to the inner side of the forearm
– Stiffness in elbow
– Pain and difficulty in making a fist
– Weakness in hands and wrists
Carpal Tunnel Syndrome
The carpal tunnel is a passageway in the wrist. Passing through this tunnel is the median nerve and the tendons that connect the fingers to the muscles of the forearm. CTS occurs when this median nerve is pinched because of swelling of the nerve, tendons, or both. CTS can be caused by sports like racquetball or handball, daily activities like sewing, typing, writing, driving, painting, etc. It is common in people who perform repetitive motions of the hand and wrist. It is most common in women aged 30-50.
Symptoms:
– Pain in the hand and wrist
– Tingling and numbness
– Weakness
– Typically, patients will wake at night with a burning or aching pain with numbness and tingling and will shake their hands to obtain relief and restore sensation.
Trigger Finger
Trigger finger is a condition in which your finger or thumb locks or catches in a bent position. The finger or thumb may straighten with a snap (like a trigger being pulled and released). In a severe case, the finger may lock in the bent position. This is caused by inflammation of the tendons in the finger. The tendon is covered by a protective sheath, which is lined with a lubricating fluid. When the tendon becomes inflamed, bending the finger or thumb may pull the inflamed portion through a narrowed tendon sheath, creating the snap or pop.
Symptoms:
– Soreness at the base of the afflicted finger or thumb
– Painful clicking or snapping when attempting to flex or extend
– Catching worsens after inactivity
– In a more severe case, the finger may lock in either the extended or flexed position and must be gently straightened with the opposite hand
Low Back Pain
The lower back bears most of the body’s weight and can be easily injured when you lift, reach, or twist. Pain in the lower back may come from the spine, back muscles, nerves, or other structures in the surrounding region. It may also radiate from problems in different regions, like the mid and upper back, a hernia in the groin, or issues in the ovaries/testicles. It may not be one action that causes pain in the back. Doing many things improperly over time, like sitting, standing, and lifting, may lead your back to be injured when you do something simple like bending down to pick up a dropped pencil.
Symptoms:
– A variety of symptoms may be felt
– Tingling or burning sensation
– Dull aching or sharp pain
– Weakness in legs or feet
– Pain may come on gradually or abruptly
Osteoarthritis
OA is the most common joint disorder. The cartilage (or cushioning) between bone joints wears away in this condition, leading to pain and stiffness. As the condition progresses, the cartilage dissipates and bone grinds on bone. Bony spurs usually form around the joint. OA most commonly affects the hands, feet, spine, and the weight-bearing joints like the hips and knees. The two types of OA are primary and secondary. Primary occurs with no incidence of injury or obvious cause. Secondary is due to another condition. Secondary OA is most commonly caused by metabolic conditions (i.e., acromegaly), problems in anatomy (i.e., being “bow-legged”), injury, and inflammatory disorders (i.e., septic arthritis).
Symptoms:
– Grating of the joint with motion
– Joint pain in rainy weather
– Joint swelling
– Limited movement
– Morning stiffness
Trochanteric Bursitis
Bursae are small, fluid-filled sacs that provide cushioning and lubrication between bones, tendons, and muscles near your joints. When a bursa becomes inflamed, this is called bursitis. It inhibits movement and causes pain in the afflicted area. Bursitis often affects the joints in your shoulders, elbows, or hips. But you can also have bursitis in your knee, heel, and the bottom of your big toe. Overuse, stress, and direct trauma to a joint are common causes of bursitis. It can also be a result of an infection, gout, or arthritis. Bursitis of the hip, or trochanteric bursitis, is frequently associated with a hip injury or arthritis. Pressure from standing or sitting for a long time is also a contributing factor.
Symptoms:
– Dull ache in the area around your hip (primarily over the greater trochanter, which is the portion of your thighbone, or femur, that protrudes where the joint meets the hip)
– Stiffness in the joint
– Increased pain with movement
– Tenderness
– Unlike bursitis in other areas of the body, there is no visible swelling or redness of the skin. This is because the bursae are located beneath some of the bulkiest muscles in the body.
Total Hip Replacement
This is a surgery performed to replace all or part of the hip joint with an artificial device (prosthesis). Physical therapy is a necessity after this procedure has been performed in order to regain flexibility and strength in the joint. The hip is a ball-and-socket joint: a meeting of the “ball” end of the thighbone (femur) with the cup-shaped “socket” of the pelvic bone. A total hip prosthesis is surgically implanted to replace the damaged bone in the hip joint.
Symptoms:
– Wearing down of the hip joint and pain because of osteoarthritis, rheumatoid arthritis, avascular necrosis,
injury, and bone tumors
– Pain that causes sleepless nights
– Difficulty walking up or down stairs
– Little or no relief from pain medications
– Difficulty standing from a seated position
– Having to stop activities you enjoy, such as walking, because you’re in too much pain
Anterior Cruciate Ligament Tear (ACL Tear)
An anterior cruciate ligament injury is extreme stretching or tearing of the anterior cruciate ligament (ACL) in the knee. A tear may be partial or complete. Ligaments are strong bands of tissue that attach one bone to another. The ACL connects the thighbone to the shin bone, crossing the knee. For an unknown reason, women are more susceptible to ACL injuries. ACL tears may be caused by contact or non-contact injuries. A blow to the side of the knee, like during a football tackle, may result in an ACL tear. However, coming to a quick stop, combined with a direction change while running, pivoting, landing from a jump, or overextending the knee joint, can cause injury to the ACL. Sports like basketball, football, soccer, and skiing have regular occurrences of ACL tears.
Symptoms:
– Feeling or hearing a pop in the knee at the time of injury
– Pain on the outside and back of the knee
– The knee swelling within the first few hours of the injury
– Limited knee movement
– Knee wobbling, buckling, or giving out
Total Knee Replacement
TKR can help relieve pain and restore function in the knee joint. The surgeon cuts away damaged bone and cartilage from your thighbone, shinbone, and kneecap and replaces it with an artificial joint (prosthesis). More than 95 percent of people who receive a TKR experience significant pain relief, improved mobility, and a better overall quality of life (from MayoClinic.com).
Symptoms that may lead one to consider a knee replacement:
– Knee pain that doesn’t respond to therapy (medication, or therapy for 6 months or more)
– Pain that limits or prevents activities
– Inability to sleep through the night because of knee pain
– Arthritis of the knee
– Decreased knee function caused by arthritis
– Some tumors involving the knee
Shin Splints
Shin splints, or medial tibial stress syndrome, is a very common condition. It is pain that runs along the shinbone, the long bone in the front of your lower leg (called the tibia). Shin splints aren’t’t a single medical condition. Instead, it’s a symptom of an underlying problem. The pain is the result of an overload on the shinbone and the connective tissues that attach your muscles to the bone. The causes are varied: flat feet, running, dancing, increased intensity of training, stress fractures (tiny hairline breaks in the bone), and a change of training surface (i.e., track to asphalt) can all be causes.
Symptoms:
– Tenderness, soreness, or pain along the inner part of your lower leg
– Mild swelling
– Weakness or numbness in the feet
Calf Strain
A calf strain is an injury to the muscles and tendons in the back of the leg, below the knee. Often called a “pulled” muscle, a strain occurs when the muscle fibers or tendons are stretched or torn. This condition can occur during any physical activity where you push off forcefully from your toes. It may occur in running, jumping, or lunging.
Symptoms:
– Immediate calf pain
– You may hear or feel a pop or snap in the calf
– Difficulty rising on toes
– Bruising and swelling may occur
Ankle Sprains
A sprain is an injury to the ligaments around a joint. Ligaments are the strong, flexible fibers that connect one bone to another. When a ligament is stretched too far or tears, the joint will become painful and swell. An ankle sprain can range from mild to severe depending on how badly the ligament is damaged. Most ankle sprains happen when you make a rapid shifting movement with your foot planted, like when playing soccer or being tackled in football. A sprain can occur in an event as simple as accidentally rolling your ankle.
Symptoms:
– Mild sprain
– Pain in the ankle
– Tenderness, swelling, and stiffness
– Bruising may occur in a more serious sprain
– Severe sprain
– Pain
– Bruising, tenderness
– Weakness, “wobbly” ankle
– Walking is not possible because the ankle gives out
– Plantar Fasciitis
Plantar Fascitis
This condition is a heel pain caused by inflammation of the plantar fascia, the tissue along the bottom of your foot that connects your heel bone to your toes. Your plantar fascia acts like a shock-absorbing bowstring, supporting the arch in your foot. If tension becomes too great, it can create small tears in the fascia. Repetitive stretching and tearing can cause the fascia to become irritated or inflamed. The band of fascia may swell and become painful. This is one of the most common foot-related orthopedic complaints.
Symptoms:
– Sharp, stabbing pain in the inside part of the bottom of your heel
– Pain in the bottom of the heel, usually worse in the morning and improving throughout the day
– Pain that worsens when climbing stairs or when standing on tiptoe
– Pain after long periods of standing or after getting up from a seated position
– Pain after, but not usually during, exercise
– Mild swelling in your heel
Adding {{itemName}} to cart
Added {{itemName}} to cart